Freiberg Disease
Frieberg disease (Alfred Freiberg, 1914) is a painful collapse (osteochondrosis) of the articular surface of the second metatarsal head. It was originally postulated that the condition was partially caused by excessive length of the second metatarsal which, when combined with an ineffective first ray complex, led to an overload of the second metatarsal and subsequent articular collapse. It has an adolescent and an adult form.
Incidence
The exact incidence is unknown. The individuals most commonly affected are adolescence females. However, it can occur at any age.
Katcherian et al., in a review of 275 cases, found an overall five times more incidence of Frieberg disease in females. In more than 95% of cases, the lesion is found in the second or third metatarsal, with the second metatarsal being affected more often. Bilateral involvement has been reported to occur in fewer than 10% of patients.
Patients usually present with poorly localised pain in the affected forefoot that is exacerbated by walking. There may be associated stiffness and a sensation of a ‘small, hard object’ under the foot.
Etiology
Freiberg disease is a degenerative process, which in its juvenile form, involves the epiphyses resulting in osteonecrosis of subchondral cancellous bone. This may be followed by regeneration or recalcification, or the degenerative process continues and results in subchondral collapse and fragmentation of the articular surface. The exact etiology still remains unknown. It is considered to be multifactorial.
Pathogenesis
Despite several theories, no consensus exists as to what type of disease process reflects its actual occurrence. Most current theories focus on the initial insult being primarily traumatic or vascular.
Vascular Theory
Radiographic changes consistent with avascular necrosis form the basis of vascular insult. It remains unclear whether this is the result of a direct vascular injury or of repetitive injury to an area with inherently poor blood supply. There is some suggested association with disorders that may affect blood supply (diabetes, SLE and hypercoagulability).
Vascular Theory
There are several studies that have reported a wide variation in the blood supply to the metatarsal heads. It is generally believed that there is less consistent blood supply to the second and third metatarsals and this could pose more risk for development of Freiberg disease in some individuals than the others.
In a cadaveric study on 200 feet, Huber described the variability of the dorsal arteries and found that 65% of those feet exhibited limited collateral anastomosis.
Leung and Wong described seven different patterns of blood supply originating from the first dorsal webspace artery.
Wiley and Thurston also noted similar variations and found that 33% of specimens studied lacked a second metatarsal artery, with collaterals from the first and third metatarsal arteries providing circulation to the second metatarsal head.
Traumatic Theory
Various authors have suggested that altered kinematics around the forefoot may predispose some individuals to a repetitive injury, abnormal loading and may ultimately contribute to the development of Freiberg disease. Smillie considered Freiberg disease to be a repetitive stress injury, similar to stress fractures.
Long second metatarsal has frequently been implicated with Freiberg disease. Stanley et al. found that the affected ray was the longest in 85% of the feet on measurement on plain standing radiographs. They noted that only five of 33 feet (15%) in their study had a discrete history of trauma. Some authors relate wearing high heel shoes to Freiberg disease however, there is no direct evidence linking the disease with shoe wear.
Classification
Smillie Classification
Stage 1 - Subchondral fracture visible only on MRI
Stage 2 - Dorsal collapse of articular surface on plain radiographs
Stage 3 - Collapse of dorsal MT head, with plantar articular portion intact
Stage 4 - Collapse of entire MT head, joint space narrowing
Stage 5 - Severe arthritic changes and joint space obliteration
Bragard Classification
Stage I - Metatarsal head flattening and decreased subchondral bone density
Stage II - Metatarsal head sclerosis, fragmentation and deformation, with cortical thickening
Stage III - Metatarsophalangeal (MTP) osteoarthrosis with intra-articular loose bodies
Imaging
Standard weightbearing plain radiographs are performed as the first line and may show changes depending on the stage of the disease. MRI is helpful in early stages and can show subtle changes and patchy oedema.
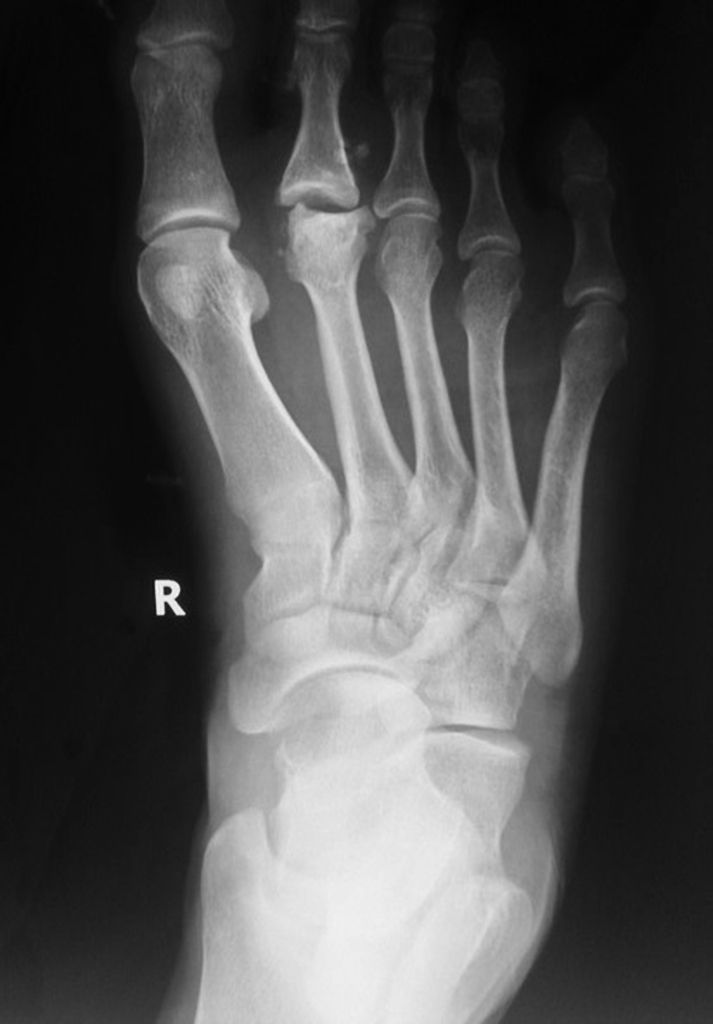
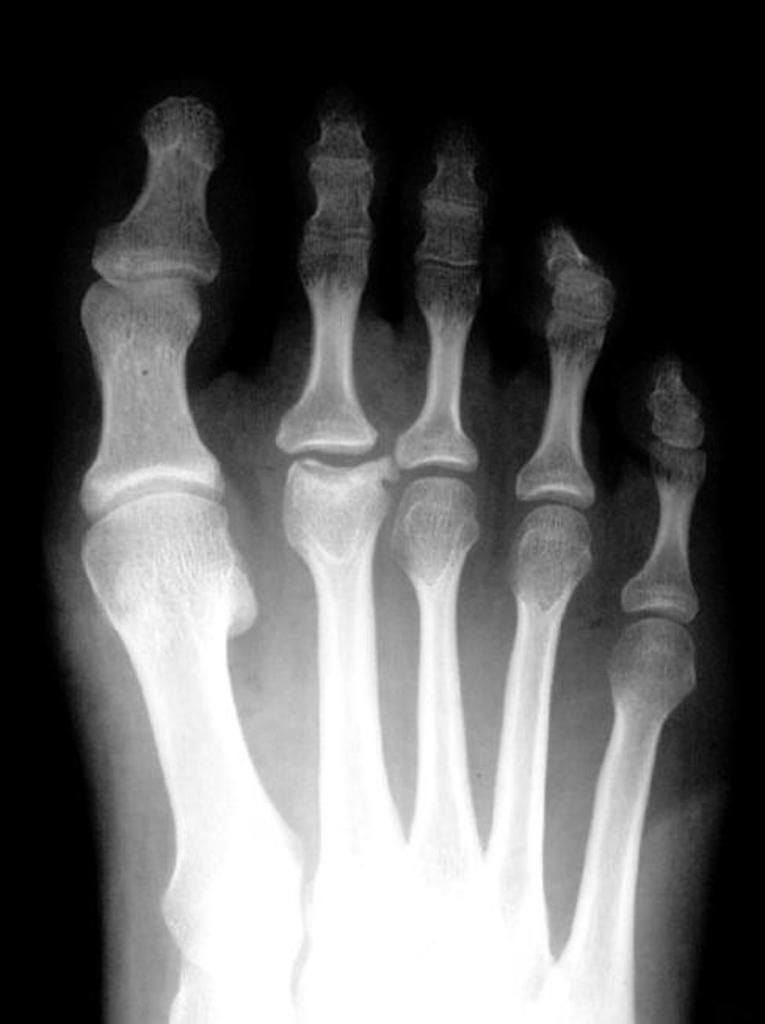
Radiographic features include:
Early
Flattening and cystic lesions of the affected metatarsal head
Widening of the metatarsophalangeal (MTP) joint
Late
Osteochondral fragments
Sclerosis and flattening of the bone
Increased cortical thickening


Treatment
Conservative Treatment
There is no clear consensus on the treatment; however, first line of treatment is always conservative. Patients with stage 1, 2 and 3 are likely to respond well to non-surgical modalities and these must also be trialled in stage 4 and 5 prior to surgery.
The aim of treatment is to rest the joint to allow inflammation and mechanical irritation to resolve.
In patients with acute and severe pain, immobilisation with a plaster cast, a walker boot or a wooden-sole shoe with protected weightbearing (4-6 weeks) provides sufficient relief.
In patients with chronic symptoms, shoe modifications with insoles, metatarsal bars, rigid shanks, or a rocker bottom, may provide symptomatic relief.
Activity modification and NSAIDs are also helpful and commonly recommended.
Hoskinson reported on the long-term results (mean 12 years) of conservative treatment on a series of 16 patients. Eleven of the 16 patients were completely pain free at final follow-up; however, all 16 had some restriction in range of motion.
Surgical Treatment
Patients who fail to respond to surgery and have persistent symptoms are considered for surgery.
Surgical options comprise a spectrum from simple debridement and excision of loose bodies to various osteotomies to achieve elevation of the depressed metatarsal head, core decompression, metatarsal head excision, shortening of the metatarsal, proximal phalanx hemiphalangectomy, total joint arthroplasty, and combinations of the above.
There is no study in literature which would prefer a single answer, as the studies report only small numbers due to less frequent requirement of surgical intervention in an uncommon condition. However the aim of surgery is to restore the joint congruency and to improve pain and function opting for the least invasive procedure.
Debridement
Some authors have advocated simple debridement as an effective treatment. However, current evidence is insufficient to make detailed assessment of results.
Erdil et al. reported their results on 14 patients with advanced-stage disease and found the debridement to be a safe, simple and effective treatment option.
Hoskinson reported 12 patients who were treated with a variety of surgical procedures, including excision of the metatarsal head (n=4), hemiphalangectomy (n=4), and debridement with loose-body excision (n=4). The best results were observed with simple debridement, however the numbers were very small to draw a sound conclusion.
Osteotomy
Several different osteotomies are practiced, however the aim is to redirect the loading of the MTP joint away from the damaged area of the articular surface. The two common types are dorsal closing wedge osteotomy and shortening osteotomy.
Dorsal closing wedge osteotomy
First described by Gauthier and Elbaz, who reported the outcomes of 53 patients in their series. The authors reported satisfactory results with no complications. In 35 of the 53 cases, the postoperative arc of motion was found to be 80° (average).
Al-Ashhab et al., in a series of 10 patients, produced good results in stage 4 and 5 disease.
Chao et al. reported results of 13 patients with all stages of Freiberg disease who were treated with dorsal closing wedge osteotomy combined with synovectomy and debridement and an average follow-up of 40 months. Based on AOFAS scores, 4 patients reported excellent results, 7 reported good results and 2 had poor or fair results.
Kinnard and Lirette reported on 15 patients who were treated with dorsiflexion osteotomy with advanced-stage disease and reported complete pain relief, with only three patients experiencing mild discomfort related to athletic activities and no complication.
Shortening osteotomy
Smith et al. described a shortening osteotomy (4 mm) and reported on 16 patients. Fifteen had complete pain relief; however, seven patients experienced some stiffness after surgery. Five patients graded their result as ‘excellent’, nine as ‘good’, one was ‘satisfied’ and one was ‘unhappy’ with the result. Two minor complications occurred; one sinus requiring re-exploration and one hardware failure. The authors described the procedure beneficial with being relatively easy, avoiding damage to the metatarsal head, and achieving possible remodelling of the articular surface.
Core Decompression
For early stage disease core decompression (using a small K-wire) has also been tried. Maresca et al. described arthroscopic drilling in a patient with bilateral stage 2 disease with some evidence of restoration of the joint surface and satisfactory results at 2 years.
Arthroplasty
Resection arthroplasty
This has gradually fallen out of favour with better options being available. If selected, this can be combined with or without soft-tissue interposition arthroplasty. The main concerns are the development of transfer lesions as a result of rendering the affected metatarsal incompetent.
Hoskinson reported the outcomes of eight patients treated with resection arthroplasty, (hemiphalangectomy and resection of the metatarsal head) and found that only three patients had a satisfactory result, while the other five had residual symptoms and deformity.
Total joint arthroplasty
Silicone prosthesis has also been tried for the treatment of Freiberg disease. Potential complications are similar to those for resection arthroplasty; with additional risks of synovitis, infection and dislocation.
Potential advantages over resection arthroplasty include maintenance of length and the range of motion with better weight distribution if condyles are preserved. There is not enough data to provide a sound evidence for these implants.
Other available options include titanium hemiarthroplasty and total ceramic arthroplasty, however their possible complications include implant loosening, bone erosion, infection, and a stiff, floating toe.
Interposition arthroplasty
As a consequence of the lack of consistent results with both resection and small-joint arthroplasty, there has been some interest in interposition arthroplasty. Unfortunately, this procedure too has yielded mixed, unreliable results.
References
-
Freiberg AH. Infraction of the second metatarsal bone, a typical injury. Surg Gyn Ob. 1914. 19:191.
-
Stanley D, Betts RP, Rowley DI, Smith TW. Assessment of etiologic factors in the development of Freiberg's disease. J Foot Surg. 1990 Sep-Oct. 29(5):444-7.
-
Cerrato RA. Freiberg's disease. Foot Ankle Clin. 2011 Dec. 16(4):647-58.
-
Huber JF. The arterial network supplying the dorsum of the foot. Anatomy Rec. 1941. 80:373.
-
Leung PC, Wong WL. The vessels of the first metatarsal web space. An operative and radiographic study. J Bone Joint Surg Am. 1983 Feb. 65(2):235-8.
-
Wiley JJ, Thurston P. Freiberg’s disease. J Bone Joint Surg Br. 1981. 63:459.
-
Bayliss NC, Klenerman L. Avascular necrosis of lesser metatarsal heads following forefoot surgery. Foot Ankle. 1989 Dec. 10(3):124-8.
-
Donahue SW, Sharkey NA. Strains in the metatarsals during the stance phase of gait: implications for stress fractures. J Bone Joint Surg Am. 1999 Sep. 81(9):1236-44.
-
Smillie IS. Freiberg's infraction (Kohler's second disease). J Bone Joint Surg Br. 1957. 39B:580.
-
Hoskinson J. Freiberg's Disease: A Review of the Long-term Results. Proc R Soc Med. 1974 Feb. 67(2):106-7.
-
Gauthier G, Elbaz R. Freiberg's infraction: a subchondral bone fatigue fracture. A new surgical treatment. Clin Orthop Relat Res. 1979 Jul-Aug. (142):93-5.
-
Goud A, Khurana B, Chiodo C, Weissman BN. Women's musculoskeletal foot conditions exacerbated by shoe wear: an imaging perspective. Am J Orthop (Belle Mead NJ). 2011 Apr. 40(4):183-91.
-
Mifune Y, Matsumoto T, Mizuno T, Ikuta S, Kurosaka M, Kuroda R. Idiopathic osteonecrosis of the second metatarsal head. Clin Imaging. 2007 Nov-Dec. 31(6):431-3.
-
Smillie IS. Treatment of Freiberg's infraction. Proc R Soc Med. 1967 Jan. 60(1):29-31.
-
DiGiovanni CW, Patel A, Calfee R, Nickisch F. Osteonecrosis in the foot. J Am Acad Orthop Surg. 2007 Apr. 15 (4):208-17.
-
Erdil M, Imren Y, Bilsel K, Erzincanli A, Bülbül M, Tuncay I. Joint debridement and metatarsal remodeling in Freiberg's infraction. J Am Podiatr Med Assoc. 2013 May-Jun. 103(3):185-90.
-
Lee SK, Chung MS, Baek GH, Oh JH, Lee YH, Gong HS. Treatment of Freiberg disease with intra-articular dorsal wedge osteotomy and absorbable pin fixation. Foot Ankle Int. 2007 Jan. 28(1):43-8.
-
Al-Ashhab ME, Kandel WA, Rizk AS. A simple surgical technique for treatment of Freiberg's disease. Foot (Edinb). 2013 Mar. 23(1):29-33.
-
Chao KH, Lee CH, Lin LC. Surgery for symptomatic Freiberg's disease: extraarticular dorsal closing-wedge osteotomy in 13 patients followed for 2-4 years. Acta Orthop Scand. 1999 Oct. 70(5):483-6.
-
Kinnard P, Lirette R. Freiberg's disease and dorsiflexion osteotomy. J Bone Joint Surg Br. 1991 Sep. 73(5):864-5.
-
Smith TW, Stanley D, Rowley DI. Treatment of Freiberg's disease. A new operative technique. J Bone Joint Surg Br. 1991 Jan. 73(1):129-30.
-
Lui TH. Arthroscopic interpositional arthroplasty for Freiberg's disease. Knee Surg Sports Traumatol Arthrosc. 2007 May. 15(5):555-9.
-
Shih AT, Quint RE, Armstrong DG, Nixon BP. Treatment of Freiberg's infraction with the titanium hemi-implant. J Am Podiatr Med Assoc. 2004 Nov-Dec. 94(6):590-3.
-
Townshend DN, Greiss ME. Total ceramic arthroplasty for painful destructive disordersof the lesser metatarso-phalangeal joints. The Foot. 2006. 17:73.
-
Miyamoto W, Takao M, Uchio Y, Kono T, Ochi M. Late-stage Freiberg disease treated by osteochondral plug transplantation: a case series. Foot Ankle Int. 2008 Sep. 29(9):950-5.
